Achilles Tendinopathy may be the Cause!
After weeks locked up at home and the cold air of winter approaching, many people are starting to feel those aches & pains creep in – a major one being Achilles pain or tendinopathy, often felt as a pain/ache/pulling sensation at the back of the heel (or nearby areas).
If you’ve been spending many hours sitting, standing or laying down, it’s very likely that this extension of your calf muscles has become a bit too tight and is creating problems for you.
In this series we will cover 4 main topics:
- What is an Achilles? What is tendinopathy?
- Why do I get Achilles tendinopathy?
- How can I treat/fix it?
- How can I stop it happening (again)?
- What is an Achilles?
While the original Achilles was a warrior in Greek mythology (portrayed by Brad Pitt in 2004’s Troy), his famous ‘Achilles heel’ is linked to the actual part of your body – a thick tendon which connects your calf muscle to the back of your heel bone.
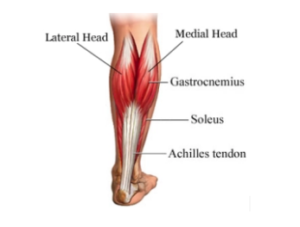
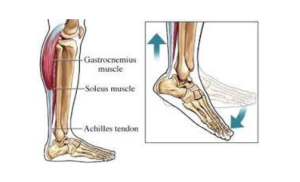
When the calf muscles contract they pull on the Achilles tendon, which then uses its grip on the heel to pull the heel back/upwards and bring the front of the foot down. You often do this when you walk, stand on your tip-toes or drive.
Tendons?
The Achilles is one of the largest tendons in the body. Tendons are tough bands of fibres which attach muscles to areas of bone. These bands of fibres act like ‘ropes’ through which muscles can ‘pull’ on bones & joints to move them (and therefore, the body).
What’s Tendinopathy?
Tendinopathy occurs when a tendon becomes damaged, inflamed or irritated – often as a result of overuse or repetitive strain. This could be anything as little as minor, sore inflammation of a small section of a toes tendon, to a large tear in the Achilles tendon.
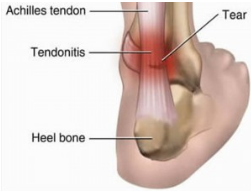
At its most severe level (eg. large tear) tendinopathy can be constantly painful even at rest, with any activity or movement of the connected muscles and joints causing terrible pain. When a large, important tendon like the Achilles is affected – it can make every step taken a painful experience.
Why Do I Get Achilles Tendinopathy?
In short – Achilles become painful because people take their poorly conditioned muscles & push them through activities they can’t handle (in their current condition. This will usually occur due to a combination of 2 main factors:
- weakness or tightness of the calf muscle
- overload /stress on the calf & Achilles tendon

Tightness can occur from overuse of the muscle without adequate rest & repair time; whereas both tightness & weakness can result from spending too much time underused & in a shortened position (eg. sitting at a desk).
If you take this tight or weak muscle, and then put a load on it which it can’t handle – this will tend to lead to tendinopathy. For the Achilles, this overload or stress can relate to:
- sudden starting or increase of activity (eg. running)
- extra pressures/load on the Achilles (eg. from Flat feet or obesity)
- environment (eg. cold = worse, hard/uneven surfaces = worse).
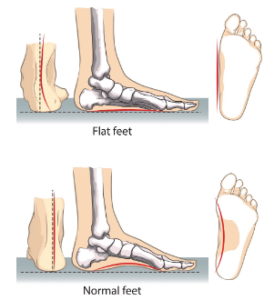
While there are other possible causes linked to Achilles tendinopathy (eg. certain antibiotics, psoriasis or high blood pressure), they are generally not the main cause.
How can I Treat/Fix Achilles Pain?
As with many pains around the foot & lower-leg area, Achilles tendinopathy (or pain at the back of the heel/ankle) is main due to 3 key factors, with 3 key things you can do to manage this problem:
- Calf tightness & weakness
- Stretches & exercises to loosen & strengthen the calf (which pulls on the Achilles at the heel).
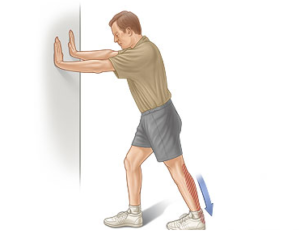
- Footwear & foot posture
- Control any Flat feet or ‘rolling in’ (or ‘out’) with proper footwear support (in the correct areas) is important.
- Activity
- Minimise sedentary postures (like sitting or standing still for too long) and reduce sudden/intense activity which can trigger (or further worsen) any ‘flare ups’ in pain.
While there are many other tips and tricks (eg. rest, ice vs. heat, foam rolling, compressions & braces) that people can utilise at home, there are some key treatments your podiatrist can perform in-clinic, including:
- Sports taping
- Massage
- Dry needling
- Shockwave therapy (ESWT)
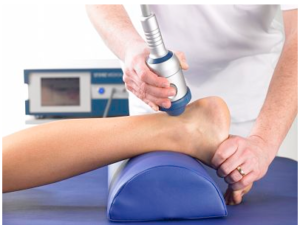
- Footwear recommendations
- Footwear modifications (eg. padding/wedging)
- Insoles / Orthotics
Most of the ‘hand-on’ therapies noted here are generally performed on the Calf muscle – and not always on the Achilles or heel itself, but either way: strain on the Achilles is reduced.
If you are searching for “Podiatrist Burwood“, you’ve come to the right place.